Indications for use of Tranexamic Acid (TXA)
Trauma
Trial Name: CRASH 2 (Positive trial)
Trial Type: Multicenter, double-blind RCT
Sample size: 20,211
Dose/Route of TXA: Loading dose 1g over 10 min, then infusion of 1g over 8hr
Primary outcome: All-cause mortality within 4 weeks of injury
Secondary outcome: Vascular occlusive events (AMI, stroke, PE, and DVT), surgical intervention, receipt of blood transfusion, and units of blood products transfused
Results: Reduced All-cause mortality p 0.0035, death due to hemorrhage p 0.0077, no significant vascular occlusion p 0.96
Risk of thrombotic events: No increase in risk
Take home point: The use of TXA in trauma patients with “significant bleeding” reduces all-cause mortality without an increase in thromboembolic events. This effect seems to be greatest in the subset of patients with severe shock (SBP ≤70mmHg) and when given ≤3 hours from time of injury
Shakur H et al. Effects of Tranexamic Acid on Death, Vascular Occlusive Events, and Blood Transfusion in Trauma Patients with Significant Haemorrhage. Lancet 2010. PMID: 20554319
Trial Name: MATTERs (Positive trial)
Trial Type: Single center, retrospective, observational study
Sample size: 896
Dose/ route of TXA: 1 g initially, 2nd dose per MD discretion
Primary outcome: 24hr mortality, 48hr mortality, and 30-day mortality
Secondary outcome: Transfusion requirements and rate of thromboembolic complications.
Results: Not significantly decreased 24 hr p >0.05, Significantly decreased 48hrs p 0.004 and 30 day mortality p 0.03
Risk of thrombotic events: Increased overall VTE p 0.001 but patients who had a VTE also had higher burden of injury
Take home point: Patients with penetrating injuries, requiring blood transfusions within 1hr of presentation the use of TXA reduced overall mortality
Morrison JJ et al. Military Application of Tranexamic Acid in Trauma Emergency Resuscitation (MATTERs) Study. Arch Surg 2012. PMID: 22006852
ICH
Trial Name: Meta-Analysis of TXA for Traumatic Brain Injury- negative trial
Trial Type: Meta-analysis and systematic review of RCTs or quasi-RCTs
Sample size: 510
Outcome: Mortality, neurological function, hematoma expansion
Results: statistically significant reduction in ICH progression with TXA non-statistically significant improvement of clinical outcomes in ED patients with TBI.
Risk of thrombotic events: No adverse effects reported
Take home point: Did not lead to a statistically significant mortality benefit or improved neurological functional status. Further evidence is required to support its routine use in patients with TBI.
Zehtabchi S et al. Tranexamic Acid for Traumatic Brain Injury: A Systematic Review and Meta-Analysis. Am J Emerg Med 2014. PMID: 25447601
Trial Name: Tranexamic Acid for Hyperacute Primary IntraCerebral Haemorrhage (TICH-2)- Negative
Trial Type: International, randomized, double-blind, placebo-controlled, parallel group
Sample size: 2325
Dose of TXA used: 1g IV TXA bolus followed by an 8hr infusion of 1g of TXA
Outcome: Functional Status at Day 90, Hematoma Expansion at Day 2, Mean Hematoma Volume Expansion from Baseline to 24hr, Death by Day 7, Death by Day 90
Results: No difference in neurological impairment (mean NIHSS score at day 7), 90-day functional outcomes, length of hospital stay, discharge disposition, venous thromboembolic events, or arterial occlusions
Risk of thrombotic events: None
Take home point: TXA was given >3hrs after stroke onset, patients had more severe strokes, and larger hematoma volumes (>60mLs) than prior studies. Possible benefit if given to a subset of patient within 3 hours with smaller strokes but cannot be recommended at this time in clinical practice for spontaneous ICH based on the results of these trials
Sprigg N et al. Tranexamic Acid for Hyperacute Primary IntraCerebral Haemorrhage (TICH-2): An International Randomised, Placebo-Controlled, Phase 3 Superiority Trial. Lancet 2018. PMID: 29778325
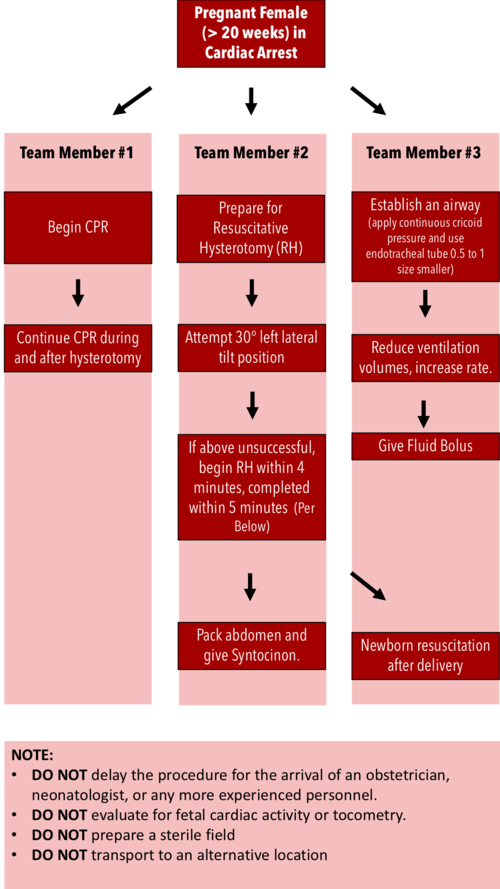
Post Partum Hemorrhage
Trial Name: WOMAN trial – Negative trial
Trial Type: Randomized, double-blind, placebo-controlled trial,
Sample size: 20,060 ≥16 years of age with post-partum hemorrhage after vaginal delivery or caesarean section
Dose of TXA used: 1 g IV vs matching placebo, If bleeding continued after 30 minutes or stopped and restarted within 24hrs, a second dose of 1g of TXA or placebo was given
Outcome: Initial outcome of all-cause mortality and/or hysterectomy within 42 days of giving birth
Final Primary Outcome: Death from PPH
Results: No difference in all cause mortality or hysterctomy
Risk of thrombotic events:
Take home point: It is difficult to draw definitive conclusions from this trial as the NNT was still large (i.e. ≈250) and the study had a fragility index of 0. Data showed a consistent association of delayed administration of TXA with no benefit
WOMAN Trial Collaborators. Effect of Early Tranexamic Acid Administration on Mortality, Hysterectomy, and Other Morbidities in Women with Post-Partum Haemorrhage (WOMAN): An International, Randomised, Double-Blind, Placebo-Controlled Trial. Lancet 2017. PMID: 28456509
UGIB
Trial Name: Cochrane review
Trial Type: Systematic review and meta-analysis of 8 RCTs
Sample size: 1700
Dose of TXA used: Total daily dose of TXA ranged from 4 – 8g and ranged from 2 – 7 days with both PO and IV adminsteration
Outcome: Primary: all-cause mortality and adverse events
Secondary: Rebleeding and surgery
Results: All-Cause Mortality p 0.007, rebleeding P = 0.07
Risk of thrombotic events: No difference in thromboembolic events (only evaluated in 4 trials)
Take home point: May benefit in higher risk patients but better RCTs required to confirm or refute evidence. HALT IT trial underway currently with N of 12000
Bennett C et al. Tranexamic Acid for Upper Gastrointestinal Bleeding (Review). Cochrane Database Syst Rev 2014. PMID: 25414987
Epistaxis
Trial Name: Zahed et al 2017 – Positive study
Trial Type: Randomized, parallel group clinical trial
Sample size: 124 on antiplatelets
Dose of TXA used: topical TXA (500mg in 5mL) or anterior nasal packing.
Outcome: Primary outcome resolution at 10 minutes. Secondary outcomes were re-bleeding rate at 24hours and one week, ED length of stay, and patient satisfaction
Results: epistaxis treatment with topical application of TXA resulted in faster bleeding cessation (NNT 2) , less re-bleeding at 1-week, shorter ED LOS, and higher patient satisfaction as compared with anterior nasal packing.
Risk of thrombotic events: not evaluated
Take home point: Do it!
Zahed R et al. Topical Tranexamic Acid Compared With Anterior Nasal Packing or Treatment of Epistaxis in Patients Taking Antiplatelet Drugs: Randomized Controlled Trial. Acad Emerg Med 2017. PMID: 29125679
Post-Tonsillectomy Bleeding
Trial Name: Meta-Analysis 2012
Trial Type: Systematic review and meta-analysis
Sample size: 7 studies with 2,444 patients
Dose of TXA used: 250mg for children <25kg, 500mg for children >25kg
Outcome: mean volume of blood loss
Results: TXA led to a significant reduction of tonsillectomy blood loss volume but had no impact on the rate of patients with post-tonsillectomy hemorrhage.
Risk of thrombotic events: Not evaluated
Take home point: In patients with minor post-tonsillectomy bleeding consider using nebulized TXA to reduce or stop bleeding.
Chan CC et al. Systematic Review and Meta-Analysis of the Use of Tranexamic Acid in Tonsillectomy. Eur Arch Otorhinolaryngol 2013. PMID: 22996082
Heavy Menstrual Bleeding
Trial Name: Cochrane Review
Trial Type: Systematic review and metanalysis
Sample size: 1312 in 13 RCTs
Dose of TXA used: majority of studies used regular dose TXA (ranging from 3 g/day to 4 g/day), Four other studies used low‐dose TXA (ranging from 2 g/day to 2.4 g/day)
Outcome: Volume of blood loss, Quality of life
Results: Appears effective for treating HMB compared to placebo, NSAIDs, Oral luteal progestogens, ethamsylate or herbal remedies but less effective than levonorgestrel intrauterine system
Risk of thrombotic events: Not studied in most RCTs
Take Home point: Antifibrinolytic treatment (such as TXA) appears effective for treating HMB compared to placebo, NSAIDs, oral luteal progestogens, ethamsylate, or herbal remedies. There were too few data for most comparisons to determine whether antifibrinolytics were associated with increased risk of adverse events, and most studies did not specifically include thromboembolism as an outcome.
Bryant-Smith AC, Lethaby A, Farquhar C, Hickey M. Antifibrinolytics for heavy menstrual bleeding. Cochrane Database of Systematic Reviews 2018, Issue 4. Art. No.: CD000249. DOI: 10.1002/14651858.CD000249.pub2
Hemoptysis
Trial Name: Inhaled TXA RCT 2018
Trial Type: Prospective, double-blind, placebo-controlled randomized controlled trial
Sample size: 47
Dose of TXA used: nebulized TXA (500mg/5mL
Primary outcome: rate of complete resolution of hemoptysis during first 5 days from admission, difference in daily volume of expectorated blood
Secondary outcome: rate of interventional bronchoscopy, rate of angiographic embolization, rate of surgery, mean hospital LOS
Results: Resolution of hemoptysis within 5 days of admission, NNT = 2, P<0.0005. Statistically shorter LOS, less invasive procedures
Risk of thrombotic events: not studied
Take home point: Although this was a small study, the advantages of inhaled TXA vs placebo in patients with non-massive hemoptysis included faster resolution of hemoptysis, shorter hospital LOS, fewer invasive procedures, and although not statistically significant, a trend toward improved 30d mortality.
Wand O et al. Inhaled Tranexamic Acid for Hemoptysis Treatment: A Randomized Controlled Trial. Chest 2018. PMID: 30321510
References:
See above
RebelEM